5 DIY Tips to Reduce Lower Back Pain
/By Mark El-Hayek, Guest Columnist
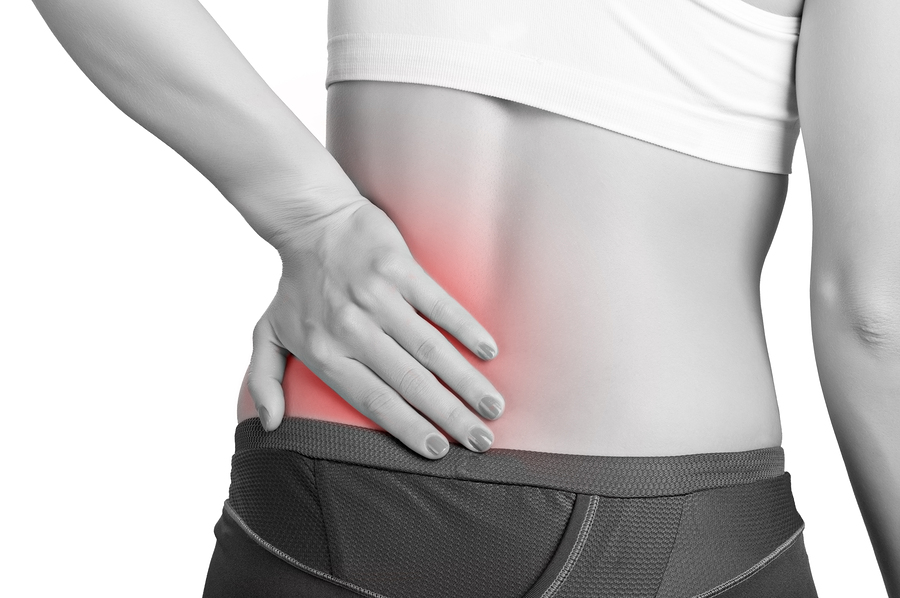
Lower back pain is the world's leading cause of disability. Almost all of us will at some point in our lives have to deal with it.
Lower back pain is any form of pain or discomfort in the lower part of the spine, which is known as the lumbar spine. It can be brought about by things like muscle tension, stress, improper diet, lack of exercise, poor posture, excess body weight and pregnancy.
We put together five simple do-it-yourself tips to help reduce lower back pain.
1) Correct Posture
Poor posture is one of the leading causes of lower back pain. Good posture involves sitting, walking, standing and sleeping in ways that do not weaken or over activate your supporting muscles. There are several things you can do to improve posture.
When sitting, avoid sitting on the edge of a chair as this puts a lot of strain on your back. Sit with your back straight and shoulders back.
The same is true for walking. Avoid bending or slouching over while walking. This strains your back and causes lower back pain.
When lying down, get into a position that is comfortable and one that does not compromise the curve in your back.
2) Ice and Heat
For many people, putting ice or something cold on an injured area provides relief from pain. Heat also works well in reducing lower back pain, but the two techniques work very differently.
When you put something cold on your lower back, the cold makes the blood vessels constrict, which reduces the pain caused by inflammation. Heat, on the other hand, relaxes blood vessels and increases blood flow, which helps heal the affected area.
It is advisable that when using ice and heat together, you start by doing the cold compress first and then the hot compress. You can use ice packs or frozen peas for the cold compress. For the hot compress, you can use a hot water bottle or a towel soaked in warm water.
Alternate between the cold and hot compresses for a few minutes and you will notice that your lower back pain has reduced.
3) Exercise
Regular exercise is a good way to prevent lower back pain. Make a point of exercising as often as you can. If you have a job that has you sitting for long hours, integrate exercises and movement into your everyday routine.
Walk to the bathroom or the water cooler a couple of times a day to keep your joints moving and lower back pain at bay. Take the stairs instead of the elevator or escalator to help stay fit.
4) Rest
Lower back pain is often caused by stress. The moment you start feeling back pain, take a couple of hours off to rest. You can start by taking a hot shower to help you relax. The shower will help your blood vessels relax and make oxygen flow freely to your lower back. After the hot shower, rest for a couple of hours and you will probably feel better.
5) Do not stay in bed too long
While resting is important, make sure you do not stay in bed too long. Lying down for an extended period of time, especially when your posture is poor or you do not have a good mattress, could increase your lower back pain. Instead of lying down, go for a slow walk to allow your joints and muscles to move and reduce inflammation.
Mark El-Hayek graduated from Macquarie University in Sydney, Australia with a Masters of Chiropractic and a Bachelor of Medical Science. He is the head chiropractor and owner of Spine and Posture Care in Sydney.
The information in this column should not be considered as professional medical advice, diagnosis or treatment. It is for informational purposes only and represents the author’s opinions alone. It does not inherently express or reflect the views, opinions and/or positions of Pain News Network.